What are spinal adhesions?
Adhesions or scarring can occur not only on the spine, but in principle anywhere inside the body. In addition to the spine, common conditions include neural structures, adhesions in the abdomen and even in the heart.
The medical term for intergrowth is adhesion. 'Adhere' means "to stick or cling to something." It refers to fibrous fibers that stick to structures or organs. Adhesions occur after surgical procedures, injuries, bleeding and inflammation. When scarring occurs after spinal interventions and disc surgeries that are basically anatomically successful, we talk about postnucleotomy syndrome. Even "healed" herniated discs leave adhesions that stick to the neural structures and print, like the herniation itself.
Spinal adhesions are consequently adhesions and scarring to the spine.
Frequency - that is what international studies say about spinal adhesions
International studies show that adhesions after operations or surgical procedures are more common than people think. Studies show that 67 percent of people who have had surgery in the past also had adhesions. The rate was 81 and 93 percent of patients who had major and multiple surgeries. For people who never had surgery, the rate of adhesions was only 10.4 percent.
The so-called postnucleotomy syndrome develops in about 15 percent of all patients who have undergone disc surgery. In two-thirds of these patients, the causes are magnetic resonance imaging-visible scarring or adhesions in the peridural space.
Causes of spinal adhesions
How do spinal adhesions develop, if not as consequences of spinal surgery? The answer is not straightforward because adhesions are one of the best-kept mysteries or riddles of modern medicine. It is even possible that people have a genetic predisposition to adhesion formation. But some facts about adhesions and scarring have been established.
Adhesions as a protective reaction
Adhesions can form because of a variety of changes (including non-surgical ones): Inflammation, injury, chemotherapy, radiation, or malignancies such as cancer can trigger adhesions. Adhesions also form after spontaneous bleeding in the epidural space, after trauma and inflammation, and after a healed disc material leak in the spinal canal. All these processes represent foreign bodies in this area. In this way, adhesions could be understood as a protective reaction.
Scarring renders the nerve roots almost immobile and also worsens blood flow and CSF circulation.
Symptoms of spinal adhesions
Often, the symptoms of spinal adhesions are moderate long-lasting pain in the leg, arm or back. A few weeks or months after the event, symptoms such as burning or pulling pain develop, often associated with discomfort in the leg or arm. Triggers for adhesions can be operations, surgical procedures, radiation or injuries.
Diagnosis spinal adhesions
Every diagnosis begins with a doctor-patient discussion. This is also the case in this situation, if adhesions or scarring are suspected.
Describe to your doctor where you have pain and for how long. Also report whether you may have had surgery on an intervertebral disc, the back in general, or even in the abdomen. Where exactly do you have pain? Is it really back pain? Based on your information, the doctor may already be able to get an idea of if any nerves are pinched.
An MRI with contrast will clearly show the adhesions in the spine. A contrast agent is a liquid. Contrast agent is designed to help scar tissue stand out more clearly from other structures on an MRI scan. This helps distinguish between a new herniated disc or adhesions.
Treatment of adhesions on the spine
One thing must be said quite clearly: There is no simple solution when it comes to the therapy of adhesions.
Can adhesions be avoided intraoperatively? The intraoperative manipulations also play a role: the more minimally invasive the procedure, the fewer adhesions will occur. Conventional procedures with larger openings are more liable to cause adhesions. Careful microsurgical dissection during surgery and avoidance of bleeding cause less scarring. Infiltration of the surgical field with anti-scar gel is useful against adhesions.
Tissue should also have time to recover and regenerate after surgery. Early stress and strain on the tissue is more likely to lead to the development of adhesions.
However, if the pain is solely due to scarring around the adequately decompressed nerve root, then there are three treatment options. These are medication, surgery, and/or psychological treatment. Before this can be done, however, a new herniated disc or instability must be reliably excluded.
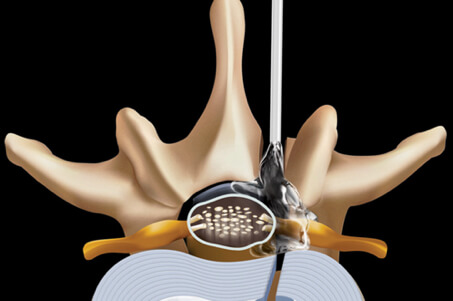
It has been shown that a careful and precise surgical technique is the most effective way to dissolve the adhesions and prevent them from forming again. The microsurgical option is the so-called adhesiolysis with the infiltration of anti-scar gel. Another procedure is epiduroscopy. With this procedure, your doctor can visualize adhesions and inflammation in the spinal canal and dissolve them with fine instruments.
Medication pain management includes a combination of pain medications. Pain management begins with simple pain medications, accompanied by physical therapy and psychosocial therapy. It is not uncommon for patients to end up with strong morphine preparations combined with antineuropathic and antidepressant substances.
A good alternative would then be spinal cord stimulation, in which electrical impulses are generated to change or suppress the pain impulses (spinal cord stimulation).
Prognosis - this is how microsurgery helps with spinal adhesions
Microsurgery is a good alternative to the removal of the adhesions. In many cases, these small procedures are sufficient to avoid the excess tissue. Anti-scar gel protects against scar development. Adequate postoperative care is important. A combined therapy as described above is often successful.
Information about the article
The article was last checked and updated on October, 25th, 2022.
About the author
Dr. med. Munther Sabarini, MD, is the director and founder of the Avicenna Clinic. As a specialist neurosurgeon, he particularly has expertise in the treatment of spinal disorders. Dr. Munther Sabarini has more than 30 years of professional experience. During this time he treated more than 30,000 patients.
Avicenna Clinic Content Quality Guidelines
All texts and content are written by medically trained, experienced experts in the field. Learn more about our content quality guidelines.
The Avicenna Clinic in Berlin is always willing to help you
Since the year 2001, the Avicenna Clinic is based in Berlin. Our doctors have at least 25 years of international experience in their respective fields (neurosurgery, spinal surgery, anesthesia, and orthopedics).
If you have severe back pain, a herniated disc or a suspected herniation, please contact us using the following information: