Pain pacemaker - what is a spinal cord stimulation?
If pain does not disappear and become chronic even after being treated with modern treatment, a so-called pain pacemaker can provide relief significantly. What is that? By spinal cord stimulation gentle impulses inhibit pain transmission to the brain. This minimally invasive surgical procedure is well established in pain therapy over more than 30 years. Several thousands of patients with chronic pain conditions are treated with this method every year in Germany.
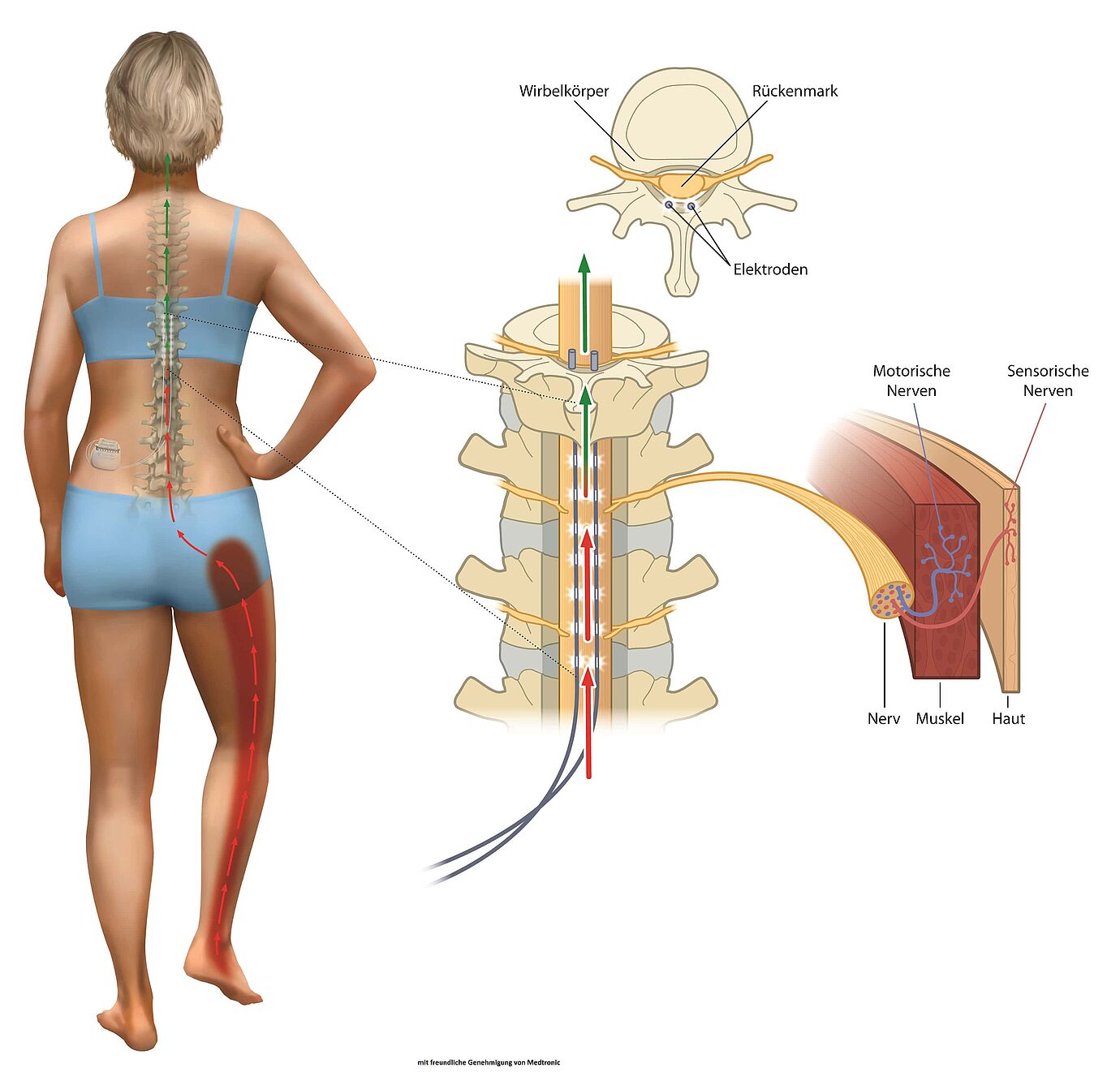
The procedure has a name: "Epidural Spinal Cord Stimulation" (SCS). It is by far the most common form of neurostimulation. The method involves introducing one or more electrodes into the epidural space through which electrical impulses are forwarded in the epidural space. The electrodes are connected to the so-called neurostimulator or neuromodulator, which is placed under the abdominal skin. The contact between the electrodes and the neurostimulator leads to the stimulation of the posterior parts of the spinal cord and the patient then notices a pleasant 'tingling sensation', exactly there, where he was feeling severe pain. In this therapy, in which the electrical impulses prevent or relieve the sensation of pain, no nerves are damaged. In addition, with a single hand movement, the patient can turn the device on and off, as well as regulate the strength in order to achieve the desired stimulation. Anyone who has ever suffered from prolonged pain knows that pain can often lead to depression - some people are no longer able to exercise their profession. The procedure SCS now makes lasting pain relief possible and gives the patient a renewed quality of life.
When is this spinal cord stimulation recommended?
This procedure is recommended in chronic pain conditions especially if conservative methods did not help. It is mostly used for pain, which exists longer as usual, accompanied by radiating pain often originated as a result of scarred changes after a disc surgery (post-nucleotomy syndrome or failed back surgery syndrome = FBSS).
The method is also effective in the so-called complex regional pain syndrome I and II (CRPS / Sudeck's disease), in peripheral arterial occlusive disease (PAOD, nerve pain because of circulatory disorders of the legs) and in the extremely painful diabetic polyneuropathy and phantom limb pain. If heart causes pain in the chest and arms, due to circulatory disorders (angina pectoris) and there are no other treatments options available, stimulation could be useful. Patients with migraine and herpes zoster (post zoster neuralgia) after being treated with spinal cord stimulation report significant pain relief and astonishing improvement in their quality of life. After incidents with nerves involvement in the arms or legs, after varicose vein surgery and inguinal hernia surgery treatment with SCS could be also recommended.
Operation procedure - pain therapy begins with an anamnesis interview
The entire procedure around this pain therapy consists of several sections. It begins with an exact neurological-orthopedic examination and an intensive and extensive anamnesis interview. We need to clarify exactly where the causes of the complaint are and if such neurostimulation could be meaningful or effective. This includes further imaging examinations such as MRI and/or CT on the spine. Of course if we find a clear reason for the pain such spinal canal stenosis or disc hernia we will try first to treat this reason. If we can foresee that neurostimulation could be helpful we will surely recommend it to you. Also in cases where we see that other surgical procedures are not meaningful or not possible we will recommend the SCS.
The next step is carried out not only to ensure your safety but also to check if this kind of stimulation is effective or not, which means: we perform so-called test stimulation. How does this trial go? This procedure is percutaneous, which means through the skin. Under local anesthesia and over a small incision at the upper lumbar area one fine electrode (or 2 electrodes) is placed in the depth on the outer layer of the spinal canal membrane using a special puncture needle. When we produce the impulses by this test you feel pleasant sensation in the pain area. In the next days after this procedure we examine (1) whether there is a significant reduction in pain through this pleasant sensation, (2) whether you take less and/or softer pain medication (3) whether you feel well and (4) whether you manage better your everyday life.
During the test, the neurostimulator, the device that later is supposed to set impulses, remains outside your body, but it is of course connected to the electrodes. We will test its effectiveness for 7-14 days in the clinic. Then you will go home for a few days and test how it works under your usual home or job conditions. If you feel clear pain relief and if you reduce your pain medication so we consider the test stimulation as successful. In this case you will be admitted again, this time for the implantation of the neurostimulator, which will produce the fine electrical impulses. If during the test phase you do not feel any improvement, we will remove the electrodes because it is not suitable for your case.
Under general anesthesia, the pulse generator - similar to a pacemaker - is implanted under the abdominal integument and connected to the electrodes and we set the generator to the level that helped you best in the test phase. After the procedure, you will receive a remote control for your stimulator, with which you can regulate the state of pain or tingling at any time. This neurostimulator is powered by a battery. It lasts a few years - when it runs out it can be replaced. Negative side effects of neurostimulation are unknown.

Benefits/Complications - the success rate of pain therapy is 85 percent!
The earlier you choose neurostimulation, the more effective will it be. In terms of numbers, 85% of patients that suffer for two years, reported good benefits after this treatment. If the duration of the pain has been more than 15 years, the success rate is reduced to just 9%. More than 50% of all patients benefit from neurostimulation. This pain therapy gives the advantage of a fast recovery, especially because it is a minimally invasive procedure. In addition, you will need to reduce the amount of pain medications. And: After being treated in the clinic you can set the intensity of stimulation by yourself.
The implant card must always be handy. You must present it if you want to pass the so-called magnetic barriers - for example, at the airport. Important: Follow the advice of your specialist and after the implantation try not to start too soon with aggressive movements because the electrodes can slip and as a consequence reduce the effect.
The Avicenna Clinic in Berlin is always willing to help you
Since the year 2001, the Avicenna Clinic is based in Berlin. Our doctors have at least 25 years of international experience in their respective fields (neurosurgery, spinal surgery, anesthesia, and orthopedics).
If you have severe back pain, a herniated disc or a suspected herniation, please contact us using the following information: