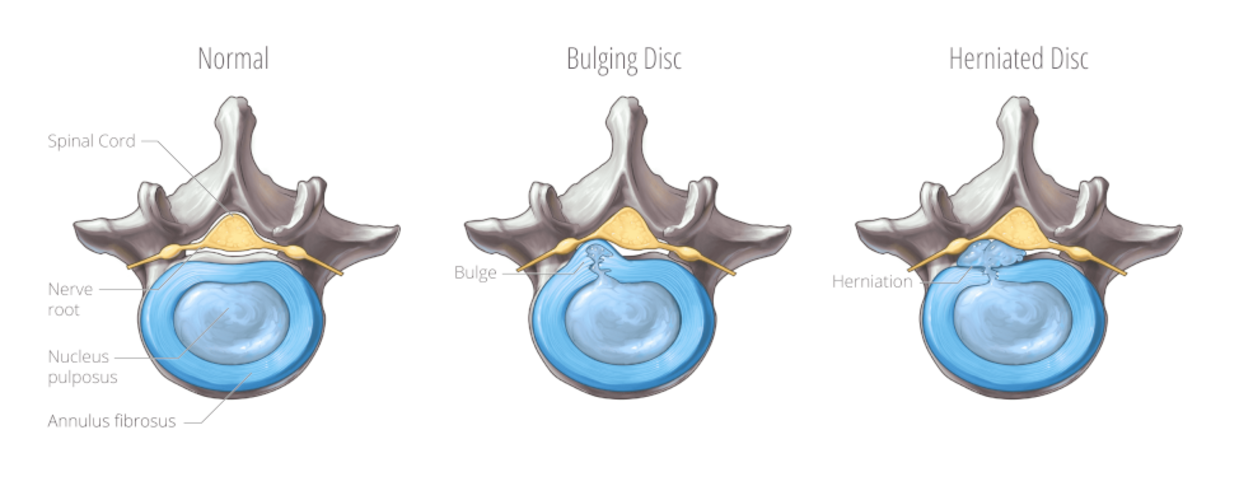
What is a herniated disc?
In the human spine, 23 intervertebral discs sit like small shock absorbers between the individual vertebrae and perform a buffering function by absorbing shocks. The discs consist of a soft, gelatinous core (nucleus) and an outer layer, the annulus fibrosus, which provides the necessary stability with its lamellae. A herniated disc (also called prolapse, sequester or discus prolapse) is a rupture of part of the disc's gelatinous core through its annulus into the spinal canal.
In the case of permanent incorrect or excessive pressure and age-related wear, there is a reduction in elasticity and small tears in the annulus. This can cause part of the gelatinous core to emerge from the ring and enter the spinal canal. In contrast to disc protrusion, the prolapsed part of the gelatinous core presses directly on the nerve root. Smaller herniated discs are referred to as prolapses and larger or more extensive ones as sequestra.
Basically, a herniated disc can occur in any area of the spine. Humans have 7 cervical vertebrae, 12 thoracic vertebrae, 5 lumbar vertebrae and one sacrum. However, most disc damage affects the lumbar spine. Medically, these incidents are also called lumbar disc herniation or lumbar herniated disc. Less frequently, damage occurs in the cervical spine (C-spine), and even less frequently in the thoracic spine.
Frequency of a herniated disc
Statistically, around 80 percent of people in Europe have occasional back pain. In Germany for example, the pain in the back even recurs regularly for around 40 percent of Germans.
A herniated disc alone is diagnosed 800,000 times a year. Patients between the ages of 45 and 55 are the most likely to receive this diagnosis.
There is no question of a fair gender distribution in the case of prolapse: Statistically, women suffer a herniated disc more often than men.
The most common causes of a herniated disc
The question of "why" comes up quickly when something painful happens to you. In the case of a herniated disc, the answer is: There are several factors that can be considered as causes for a herniated disc.
Behind a herniated disc is usually years of age-related wear and tear on the disc. It's no secret that the older you get, the older the disc gets. This is not necessarily good for the disc: it becomes less elastic and less able to store water. This increases the risk that the fibrous ring of the intervertebral disc will burst, leading to a herniated disc.
In addition to age-related wear and tear, there are a number of other causes that can lead to a herniated disc:
Wrong sitting posture
Do you sit at your desk a lot in the office? Then please pay attention to the correct sitting posture. Don't sit at your desk for hours, possibly with a cramped, hunched back. Instead, get up in between, walk, take standing breaks, relax. Make sure your office chair allows you to place your feet flat on the floor. The angle between the upper and lower leg should be about 40 degrees.
Untrained back muscles
Trained back muscles prevent herniated discs. Take advantage of back training offers. However, you can also do a lot yourself without a special back trainer. Swimming, for example, is a good preventive measure, as is cycling. Regular loading and unloading through varied movement of the back keeps the muscles and intervertebral discs healthy; insufficient or one-sided movement weakens the muscles and intervertebral discs.
Overweight & wrong nutrition
Having an overweight changes the shape of the body and thus promotes a wrong load. But being overweight as a cause is not exclusively about too many kilos. It has been proven that the spine is built to carry incredible loads.
What you should seriously consider: Overweight is usually the result of a wrong nutrition. This results the spinal discs not being adequately supplied with important nutrients. In comparison, a responsible eating regimen can significantly improve the supply of nutrients to the intervertebral discs. If the intervertebral disc is not sufficiently supplied with nutrients, the disc cover can become fragile.
Wrong lifting
Lifting incorrectly can always be a cause of a herniated disc. But how do you lift heavy objects correctly? Some back experts in physiotherapy recommend making your back completely round when lifting and going back up, vertebra by vertebra, as you lift the load. This way, muscular problems are not amplified and solidified because the back is in motion.
Other back specialists recommend getting as close to the object as possible when lifting and pushing the bottom up when bending over. They say it's important to hold the object as close to the body as possible - holding the object too far from the body increases back strain. Regardless of which variation you choose: Do both gently, slowly, no jerky lifting. And if you feel overwhelmed as a sufferer, ask someone to help you.
Smoking
Although smoking, back pain and vertebral bodies are not related at first glance, there is a connection - and it's in the brain, as American researchers found. Smoking affects the way the brain reacts to back pain. According to the study, smokers are less resilient. That is the reason why smokers suffer three times more frequently from chronic back pain than non-smokers and often also suffer a herniated disc. This is explained in the advice brochure "Strengthening the Back - Relieving Pain" published by the German Rheumatism League.
Spinal column changes
Vertebral fractures, inflammatory diseases or tumors can seriously change the statics of the spine. Therefore, such a change around the spinal canal can also be a cause of a herniated disc.
Genetics
Genes also play a role as a cause and can promote a herniated disc, especially for younger people. If there is already a family history of herniated discs, i.e. known incidents, the patient should make even more intensive efforts to maintain a healthy posture. A congenital weakness of the connective tissue can also be the cause.
The symptoms of a herniated disc - how does a prolapse become apparent?
If the herniation causes severe irritation of the nerve roots, various symptoms occur depending on the location of the herniated disc. Sometimes a herniated disc also announces itself in advance. This means that anyone who has had severe pain in the lower back for more than a week, possibly radiating into the leg and arm, should definitely see a doctor and think about therapy. Important: If in doubt, seek medical advice too early rather than too late!
We know three types of herniated discs:
- The herniation in the lumbar spine, where symptoms are usually caused by herniated discs between the fourth and fifth lumbar vertebrae (L4/L5) or between the fifth lumbar vertebra and the first coccygeal vertebra (L5/S1)
- the prolapse in the cervical spine
- and the prolapse in the thoracic spine.
Symptoms often originate in the lumbar spine, because the body weight exerts particularly strong pressure on the vertebrae and the intervertebral discs here. In the case of a herniated disc in the lumbar spine, there is usually stabbing pain in the lower back with radiation into the leg. Numbness or sensory disturbances, such as formication and tingling, can then spread to the foot. Any movement aggravates the pain, which is why the patient adopts a protective posture. Sneezing and coughing also increase the pain in the back. The muscles that support the spine reflexively harden and feel stiff. In the case of a herniated disc that extensively fills the spinal canal, there may also be pain, numbness and paralysis in the legs and also severe disturbances in bladder and rectal function. In this case, numbness occurs in the anal and genital areas, as well as on the inner side of the thighs. In case of paralysis symptoms or bladder emptying disorders, a clarification and an acute treatment must be realized immediately! The specialists of the international spine clinic in Berlin are very experienced in diagnosis and therapy.
The herniated disc in the cervical spine (C-spine) is often accompanied by neck pain radiating to the shoulder blades as well as the arms. In addition, numbness may begin in the arms and fingers. Headaches, concentration disorders, dizziness, tinnitus, disturbances of balance or visual disturbances also occasionally occur. Muscle weakness, paralysis or signs of paralysis in the arms again indicate a more severe herniated disc.
In the thoracic spine, a herniated disc is rare. Symptoms can be back pain, which usually radiates to the side. Frequently, an acute heart attack must be ruled out in the case of such pain radiation.
All types of herniated disc are associated with tension, reduced strength, restricted mobility, paralysis and sleep disturbances.
The diagnosis - how can we prove a herniated disc?
The diagnosis already begins during the doctor-patient consultation (anamnesis). Patients describe their complaints in detail.
Important questions your doctor may ask include:
- What complaints do you have? Where exactly do they radiate - to the leg or arm?
- How long have the complaints been present? What has triggered the complaints? Does the pain increase when you cough, sneeze or move around, for example?
- Can you sleep at night? Do you have problems urinating or defecating? Do you fall over? Do you sometimes stumble? Do objects fall out of your hand? Do you have tingling or numbness? Has there been any change in concentration, bladder function, vision?
- Have any therapies been used for the disc or to relieve back pain or neck pain? If yes, which ones?
After the interview, the patient goes to the neurology department, because a thorough neurological examination is necessary. For this purpose, the doctor checks reflexes, sensitivity, mobility and possibly nerve conduction velocity. Depending on whether and where the pain radiates, the doctor can draw conclusions about the level of the spine at which a herniated disc is present.
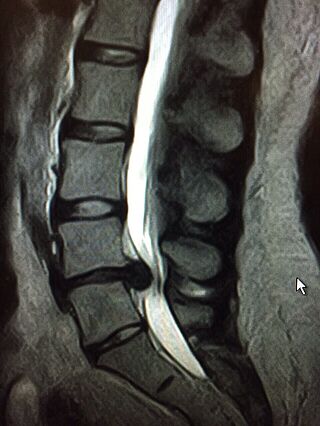
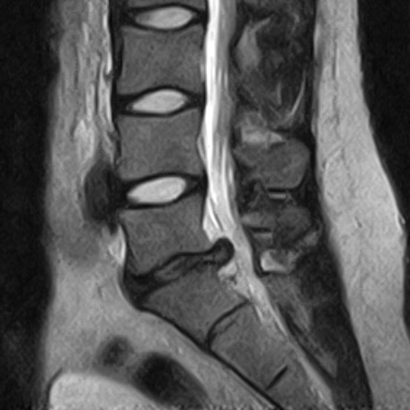
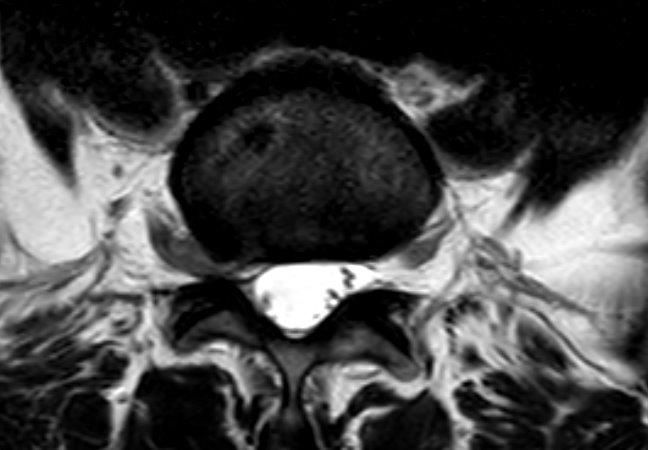
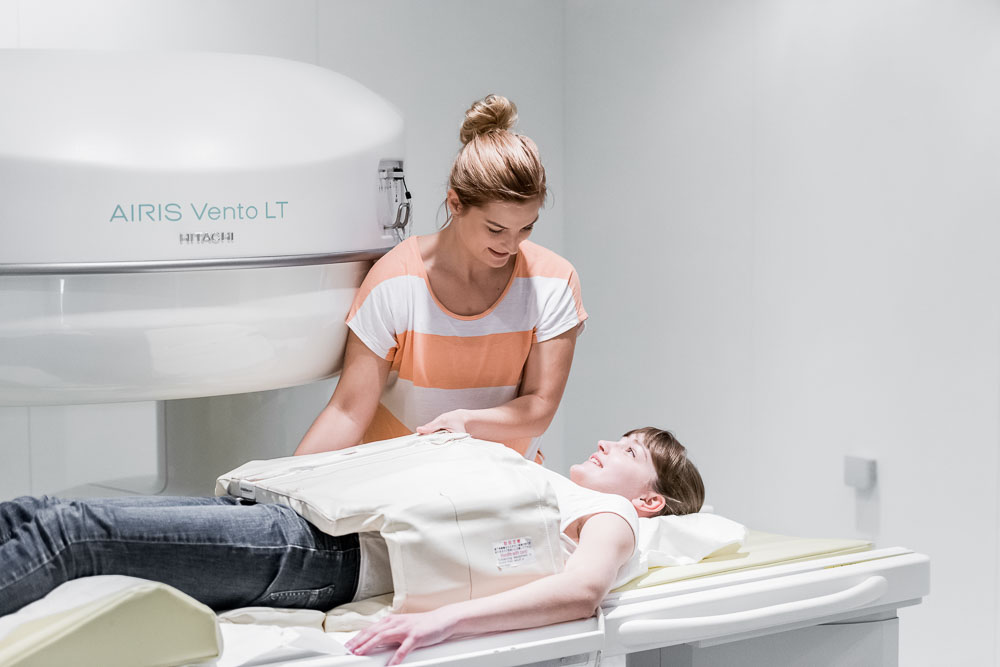
Dr. Munther Sabarini: "Occupational and psychosocial circumstances are also taken into consideration during the medical history. A magnetic resonance imaging (MRI) shows the specific changes: Herniated disc, its size and exact location, the presence of osteoarthritis, wear, instability and changes in the neural structures (myelopathy) and gives us other important information."
What treatment is appropriate to relieve or stop the disc herniation symptoms?
Deciding what therapy to recommend for a herniated disc is a big responsibility and must be made based on the following factors:
- Complaints: Pain, discomfort, loss of strength and/or bladder emptying problems.
- Success of previous therapies and duration of success, side effects of administered medications.
- General condition of the patient: severe heart disease, blood thinners?
- Neurological findings: are there sensory disturbances, reflex abnormalities, motor deficits or atrophy?
- MRI findings: small or large prolapse accompanied by tightness, instability?
- Psychosocial factors, occupation, career, care.
Based on these factors, the advantages and disadvantages of various treatment options and interventions are explained in detail. A clear recommendation can then be made as to which treatment approach should be considered. The therapy should not only relieve the symptoms, but also eliminate the cause. Ultimately, the goal is to provide lasting relief from pain and to prevent further permanent irreversible nerve damage.
Different approaches to the treatment of herniated discs
- Conservative therapies: medication, injections, computed tomography (CT) - controlled injections, infusions, physiotherapy, manual therapy, osteopathy, electrotherapy, and others;
- Minimally invasive procedures such as percutaneous laser discus decompression (PLDD) or percutaneous nucleotomy (PN) in cases of small disc hernia;
- Microsurgery for moderate and huge herniated discs especially when it is accompanied with spinal canal stenosis;
- An anti-scar gel is used against possible adhesions;
- For a herniated disc recurrence, the split of the fiber ring (fibrous annulus) is closed with a special suture technique;
- In case of an intervertebral disc cell transplantation the volume of the intervertebral discs and its elasticity are restored - by a biological regeneration of intervertebral disc tissue;
- Especially in the cervical spine, the disc can be replaced with a disc prosthesis or with a cage;
Which of all these and other methods is suitable in your case will be discussed with you individually during the consultation with the doctor. If surgery is necessary, he will discuss exactly which disc surgery is suitable for you.
Prognosis and prevention to a herniated disc
There are no guarantees on how you will prevent the herniated disc. But there are sensible measures you can take to strengthen your back and thus reduce your risk of a herniated disc. In other words, wisely live a daily routine that is kind to your back. Strong back muscles and avoiding heavy stress on the spine are the most important factors in preventing a herniated disc. Here are a few tips to help prevent a herniation:
- Pay attention to your body weight. Overweight puts additional strain on the back and vertebrae.
- Always lift heavy objects from a squatting position with your back straight.
- Get active. Gymnastics and sports strengthen the back muscles and relieve the spine. Swimming, for example, is one of the back-friendly sports, and if you like cycling, raise the handlebars.
- Pay attention to your mattress. Make sure you don't remain in an awkward position at night. Basically, after seven years, a mattress is worn out.
- If you have a job that requires you to sit a lot, do two things. Make sure you sit on an ergonomic chair with height-adjustable seats. Don't sit for hours at a time. Get up every now and then, walk a few steps, stretch. You'll be doing your intervertebral discs a big favor.
What should you do after a herniated disc?
It used to be the case that herniated disc patients should not move and had to stay in bed. Today, this is only true in rare cases.
That's why today patients start immediately with physiotherapy and various procedures to strengthen the tissues and muscles. Physiotherapy exercises relieve the spine, massages, aqua gymnastics and back-friendly sports are helpful. In this way, you prevent back pain and neck pain and relieve the strain on your intervertebral discs.
Of course, movements that strain the back and intervertebral discs are taboo. So you should not lift or carry heavy loads, do not clean in a stooped position or shovel sand after disc surgery or disc surgery.
How do I know if I have a herniated disc?
A herniated disc is particularly noticeable through pain and neurological impairments. Depending on the severity and position of the herniated disc, very different symptoms can occur: From stabbing and burning pain, tingling in the arms or legs to paralysis and numbness, the spectrum of a herniated disc ranges. If you experience any of these symptoms, we strongly advise you to visit your doctor.
Can a herniated disc disappear on its own?
Yes, a herniated disc can usually heal on its own. Surgery is by no means necessary in every case. Instead, conservative therapies can be used to support the body's natural healing process, improve mobility and relieve pain.
Can you have multiple herniated discs at the same time?
Particularly in the lumbar spine, it is possible for several herniated discs to occur at the same time or in quick succession. The first herniated disc causes instability of the spine, resulting in increased stress and misalignment of adjacent vertebrae. As a result, further herniated discs may occur.
What should you not do if you have a herniated disc?
A herniated disc is a great strain on the body: The mobility of the spine is severely restricted and pain is a constant companion in everyday life. Some movements, stresses and activities should now be urgently avoided. You should not do this with a herniated disc:
- SSports activities related to rotary movements, such as golf, skiing, tennis, badminton or squash
- Sports with impact movements for the spine: these include ball sports, running and horseback riding.
- Strength training that challenges the abdomen or back by twisting or rolling up (situps, crunches).
- Sitting for long periods of time should also be avoided. Change position and posture more often.
Where does it hurt with a herniated disc?
Where exactly the pain occurs in a herniated disc is dependent on the position of the prolapse. Depending on the section of the spine, different nerves are constricted that run in different areas of the body. In this way, the pain or neurological impairment associated with a herniated disc radiates outward and cannot be confined to one region of the body.
Information about the article
The article was last checked and updated on August 18th, 2022.
About the author
Dr. med. Munther Sabarini, MD, is the director and founder of the Avicenna Clinic. As a specialist neurosurgeon, he particularly has expertise in the treatment of spinal disorders. Dr. Munther Sabarini has more than 30 years of professional experience. During this time he treated more than 30,000 patients.
Avicenna Clinic Content Quality Guidelines
All texts and content are written by medically trained, experienced experts in the field. Learn more about our content quality guidelines.
Sources and further literature
Dt. Ges. f. Orthopädie und orthopäd. Chirurgie + BV d. Ärzte f. Orthopädie (Hrsg.): Leitlinien der Orthopädie. Dt. Ärzte-Verlag, 2th edition, Köln 2002.
Jürgen Krämer, Robert Krämer & Jörg Herdmann: Mikrochirurgie der Wirbelsäule. Georg Thieme Verlag KG, 6th edition, Stuttgart, 2005.
H.M. Mayer., F.C. Heider. Der lumbale Bandscheibenvorfall. Orthopädie und Unfallchirurgie, Georg Thieme Verlag KG, Stuttgart, 2016.
R. Krämer: Bandscheibenbedingte Erkrankungen. Georg Thieme Verlag KG, 6th edition, Stuttgart, 2013
H.S. Füeßl: Wie sich ein Bandscheibenvorfall ohne Operation zurückbildet. MMW-Fortschritte der Medizin, 158(12), Springer Medizin, 2016.
K. Schmieder: Der lumbale Bandscheibenvorfall – Spontanverlauf, Therapieoptionen und klinische Ergebnisse. Die Wirbelsäule, 3(02). Georg Thieme Verlag KG, Stuttgart, 2019
The Avicenna Clinic in Berlin is always willing to help you
Since the year 2001, the Avicenna Clinic is based in Berlin. Our doctors have at least 25 years of international experience in their respective fields (neurosurgery, spinal surgery, anesthesia, and orthopedics).
If you have severe back pain, a herniated disc or a suspected herniation, please contact us using the following information: