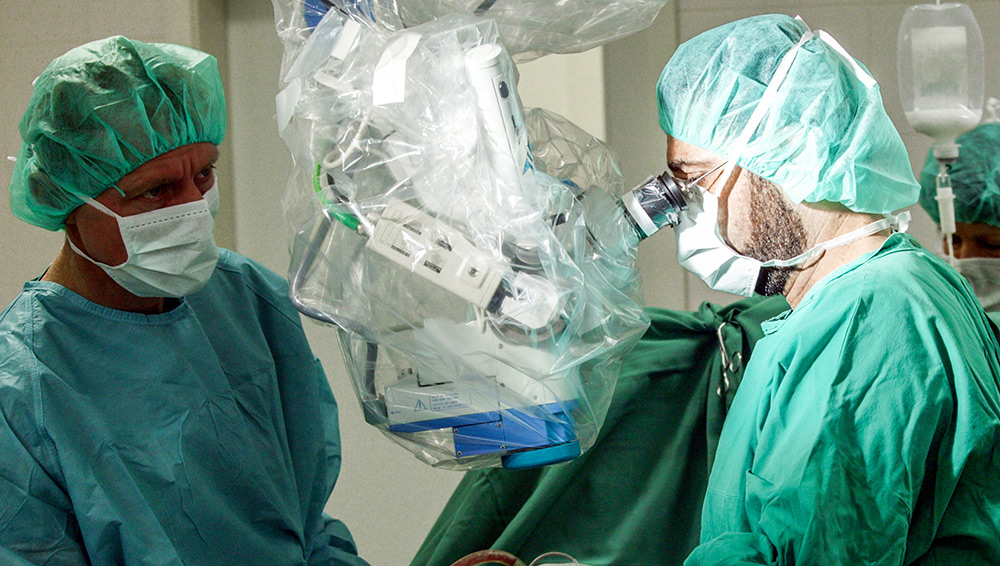
Microsurgery - it significantly reduces the risk of subsequent adhesions
Patients who require surgery will breathe if the surgeon tells them that they are undergoing microsurgical surgery. Microsurgery (from Greek μικρός, 'small') is a surgical technique that employs the use of a light microscope or other high magnifying vision aid. Special instruments allow cuts and sutures in areas that are hard to reach because of their small dimensions. This means that, in contrast to the conventional operation, the point of access will be of a few centimeters. This significantly reduces the risk of subsequent adhesions. Tissues and muscles can be protected and not damaged. In addition, unlike the major surgery, the patient recovers fast.
Microsurgery, which was first performed in 1922 by the Swedish physician Gunnar Holmgren, became a gold standard, because it helps patients to achieve lasting pain relief. The most important instrument in addition to the micro instruments is a high-performance surgical microscope, which gives an optimally illuminated, three-dimensional view into the surgical area. The nerves, vessels and the incident as well as the intervertebral disc are clearly recognizable, worn intervertebral disc parts can be removed, and constricted nerve roots can be freed.
Why is microsurgery involved when it comes to herniated discs and spinal canal stenosis in the lumbar spine?
Disc herniation and spinal canal stenosis are good reasons to make microsurgery. A herniated disc is a breakthrough of the nucleus of an intervertebral disc through its fibrous ring. As a result, he can press on nerves and trigger pain.
Each of our 23 intervertebral discs is made of an inner nucleus called the nucleus pulposus, which acts as a kind of gel cushion. This is surrounded by a hard fibrous ring (annulus fibrosis), which holds the disc in its position. If the gelatinous nucleus breaks through the fibrous ring it causes a herniated disc (prolapse / disc prolapse). With microsurgery we remove the herniated disc and relief the nerve root.
We face a spinal stenosis when the “channel” of the spine, in which the spinal cord runs, is narrowed. Pressure on the spinal cord, nerves and blood vessel causes pain and can also cause permanent damage to the nerves. The microsurgical enlargement of the spinal canal is a very effective and safe method to apply. Surgery usually brings immediate improvement.
We also use microsurgery for cysts, syringomyelia and spinal tumors.
Operation procedure - disc prolapse is prompt, stenosis develops slowly
Basically: The herniated disc is usually an acute event, stenosis on the other hand develops slowly but both cause pain. The main purpose while treating a spinal canal stenosis is to enlarge the spinal canal in order to give more space to the nerve roots. This is made with the help of tiny instruments that benefit a precise and successful treatment that will protect the spinal structures from any kind of damage. In the herniated disc (disc prolaps), the outer fibrous ring of the disc has torn and has pushed out a portion of the nucleus. Here, microsurgery allows us to remove the prolapsed disc tissue, because it can cause severe pain, damage the nerves and as a consequence could cause paralysis and numbness. This back surgery is made with a three-dimensional microscopic process of removal. Patients lie under general anesthesia, and the procedure starts with a small skin incision.
The microscope gives us an enlarged and sharp view of the nerve canal, and having a great view we can identify the anatomical structures and remove, with special instruments (forceps), the escaped disc tissue that has irritated the nerve. If the fibrous ring has closed again by itself, we remove only the prolapsed material but if the fibrous ring is still open, then we can close it with a new seam technique (closure of fibrous ring). In a stenosis, we remove the thickened structures and calcifications. Against adhesions, we infiltrate the surgical field with an anti-scar gel. Then we put drainage and close the wound.
Right after the operation
Slowly and under supervision, you will come back to the recovery room, where your health conditions will be monitored. After that our staff will bring you to your room, where you will continue to be subjected to check-ups. You must lie down on your back. On this day also begins the first physiotherapeutic treatment. Light painkillers are given after surgery. For thrombosis you wear medical thrombosis prophylaxis stockings (MTPS) and you will receive an injection daily (heparin preparation).
Post-operative days
In the next days after the operation you will be mobilized according to an individual program. When, how often and how long you can get up, walk and sit will be determined according to the healing course and your general health conditions. You receive daily physiotherapy and light pain therapy. These days, all questions are discussed: how to proceed with physiotherapy, outpatient or inpatient, stress, sports, travel, disability, sexual intercourse, further investigations and other questions that are answered individually. This depends on the patient's age, severity of findings, intraoperative features, your socio-occupational environment, comorbidities, care after discharge and other factors.
After microsurgery, you are usually 'back to life' with your usual everyday activities.
The Avicenna Clinic in Berlin is always willing to help you
Since the year 2001, the Avicenna Clinic is based in Berlin. Our doctors have at least 25 years of international experience in their respective fields (neurosurgery, spinal surgery, anesthesia, and orthopedics).
If you have severe back pain, a herniated disc or a suspected herniation, please contact us using the following information: